The pandemic's frontline: soldiers of a new kind of war
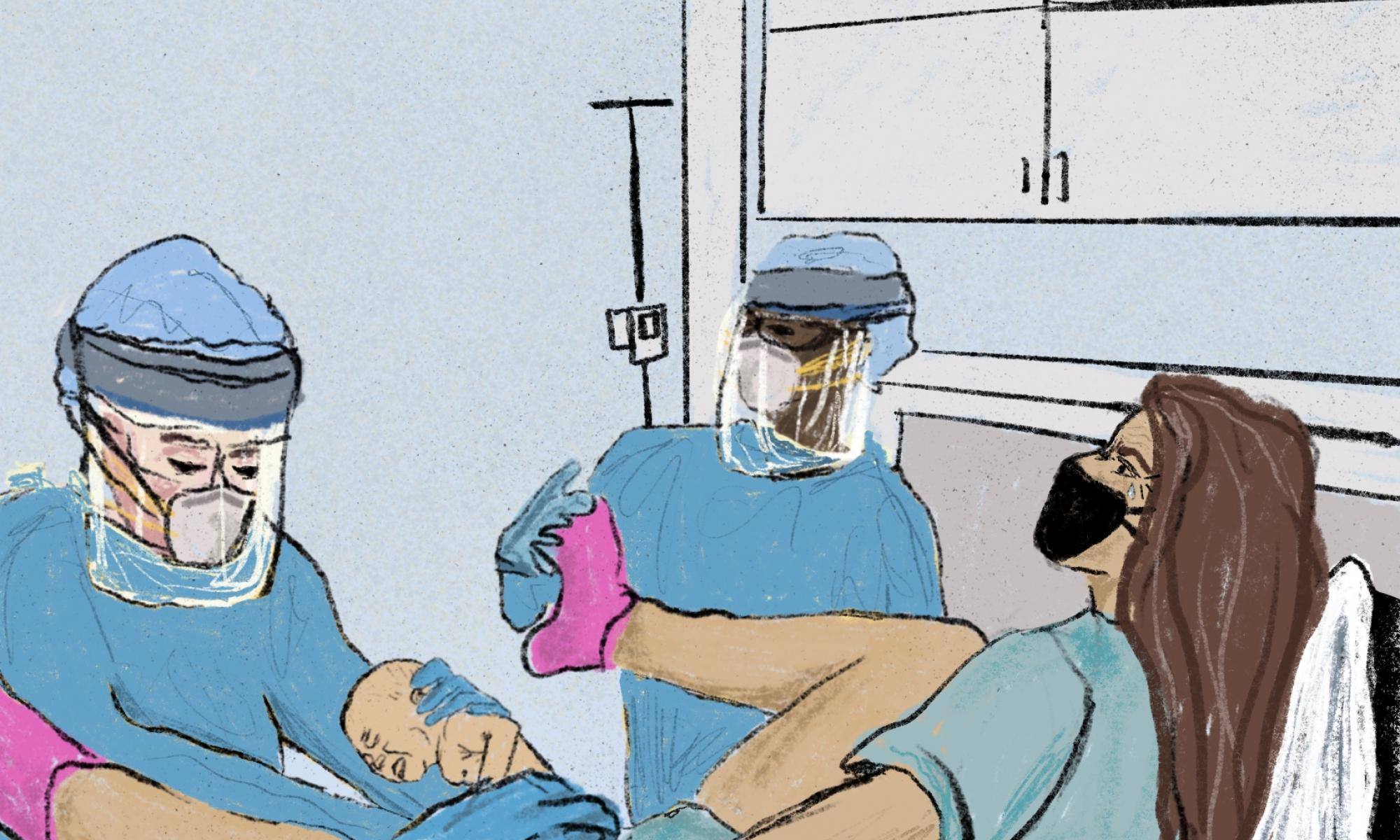
Obstetrician and gynaecologist Deborah Goldfischer has been guiding women through the birthing process in the midst of a global pandemic.
While much of the population has hunkered down to avoid exposure to COVID-19, employees in professions deemed "essential" have continued to face the outside world and its risks.
On a daily basis, doctors, health officials, and grocery store workers—to name only a few—wade into the unknown. Workers in these occupations have been tasked with keeping the world running while many of its inhabitants hold still. Below are the stories of just a few everyday soldiers in the fight against a public health crisis unlike anything yet seen in the modern era.
Deborah Goldfischer, OB-GYN | Morristown, New Jersey, US
Dr. Deborah Goldfischer was in medical school when the AIDS epidemic hit. But COVID-19, she says, is a battle unto itself. An obstetrician-gynaecologist with admitting privileges at Morristown Memorial Hospital in New Jersey, Goldfischer describes working through the pandemic as a demanding and largely disordered experience. While other doctors were asked to set aside their specialties and work with COVID-19 patients, she remained on the same service as childbirth cannot be delayed in the same manner as other elective surgeries.
"It was just chaos," Goldfischer says of the first few months. With limited knowledge of the disease and a scarcity of protective materials, standard medical protocols became blurred.
"Somebody was making it up," Goldfischer said of the new rules of patient care, "and you weren’t even sure who was making it up.”
At the start of the pandemic, New Jersey was one of the hardest-hit states in the US and Goldfischer says the hospital began asking doctors to reuse N-95 masks, a desperate measure unheard-of before COVID-19. Since personal protective gear was so sparse the safety protocol with patients would change by the hour which further confused staff. Goldfischer explained how many doctors stopped returning home to their families as consensus grew that it was not a question of if health workers would contract the virus, but when. Goldfischer herself continued to live at home as did her husband who is also a physician and therefore at equal risk. It didn't make sense for either of them to relocate, she said.
Guiding women through the birthing process can be a complicated task under any circumstances, but in the context of a global health crisis, it is doubly difficult. "They’re labouring with their masks on," Goldfischer explains, "it was very hard to comfort the patients because it wasn’t comfortable."
One patient tested positive for COVID-19 shortly before needing to have a C-Section. Since the virus is spread through bodily fluids, delivering the baby safely involved an hour long discussion over which operating room to use and how much protective gear would be necessary. Now that infection rates have slowed locally and personal protective equipment is more readily available, Goldfischer is breathing a cautious sigh of relief. "Until this is over, it’s not going to be the same," she warns, "I don’t think people realise it’s serious, we still don’t have a cure. And even these people that are getting better, they’re finding they could have these long term problems from it. It doesn’t completely go away and I don’t think people really understand that because you’re not seeing it every day in the hospital that people are really getting sick.”
Monica Scrobotovici, Healthcare, Public Health Intelligence and Improvement Manager | Grays, Essex, UK
"If anyone ever asks me what I do for a living, it’s read," Monica Scrobotovici jokes. She works as a public health officer for the Thurrock Council in Essex, east of London and was redeployed from her usual projects to respond to the coronavirus pandemic. After joining the Public Health Leadership Group, Scrobotovici's job shifted to compiling data on capacity and demand and looking at the impact her community was seeing on hospitals and care homes. Business as usual completely paused and she started working extra hours to meet the urgency of the moment.
"We get constant emails from our director with new regulations, new policies, new research findings," Scrobotovici explains. "Sometimes studies are not necessarily finding the same results so you have to make sure you follow the right ones, and considering that processes have been kind of hurried, there [are] no peer-reviewed actual studies that have been coming out so you have to kind of make your own judgment about whether something has been done properly and you should trust the results."
It's difficult to separate work from home life, Scrobotovici says. She's been lucky enough to work from home but hasn't seen her partner, who is based in the US, for over four months. Though the separation takes a toll, it has allowed her to dive further into work and in the meantime, she is safeguarding her mental health by exercising, sunbathing in the garden, and reading as much as she can—before the data changes and she needs to read it all over again.
Christian Felter, Paramedic | Alameda County, California, US
Chris Felter starts his day at 5 am, and it doesn't end until 14 hours later, give or take. Felter is a paramedic in Alameda County, a section of California serving about 1.6 million residents. He responds to an average of nine calls a day, travelling up and down the county to deliver patients to the hospital before getting back on the street where there is almost always another call waiting.
“Not just with COVID but with protesters as well, multiple streets have been shut down," Felter says, "then pretty much everyone's calling for any illness, but when you’re getting on scene there's a lot of worry from the public on going to the hospital. I wouldn’t wanna be in the hospital if I was over 55 and have co-morbidities."
Not all calls are COVID-related, of course, but paramedics are wearing personal protective equipment anyway. That means an N-95 respirator mask, glasses, and a gown. Felter says either he or his partner will don the protective gear and make patient contact, bringing them outside and putting a mask on them as well. A lot of calls that would normally be classified as general illness are being tagged now as COVID-related. The only way to know for sure is to track individual cases in the system, which Felter has done and found two confirmed positive cases among patients he's been in contact with.
"Mentally, every patient's different," Felter says of approaching the situation, "but they’re gonna get the best care I have. I’m wearing my proper PPE, so it doesn’t really affect me mentally too much, whatsoever. I’m washing my hands, I'm wearing gloves. I mean, all things considered, I would think the Safeway [grocery store] employees are a little bit more at risk than I am."
Along with the protective measures, Felter and his colleagues have been keeping a distance from friends and family outside of work. "A lot of Zoom conversations," he says of the contact he has with those outside emergency medicine, “you worry for family and friends.”
Joyce Smith, Bookstore Owner | Cincinnati, Ohio, US
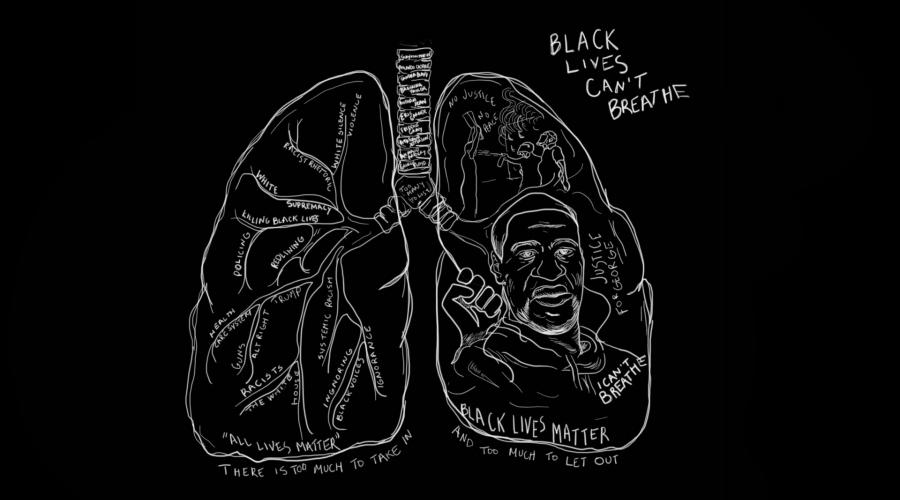
Joyce Smith is both the owner and sole employee at Smith & Hannon Bookstore. She's a frontline worker fighting what is being called the second deadly pandemic facing America—the plague of racism and white supremacy.
The killing of yet another unarmed Black man, George Floyd, by Minneapolis Police sparked widespread protests across the nation. Activists and citizens alike took to social media to encourage Americans to do their homework on uncovering oppression, knowing one's own history, and understanding the way in which they are personally complicit. This heightened awareness and the subsequent hunger for change has driven a surge in the demand for Black literature across the country.
"My bookstore is not like one of these big stores, it’s just a neighbourhood store," Smith says, "I meet the demand as best I can, I don’t have people waiting." Most orders have been coming over the phone, she says, making it easier to take care of the influx of requests. "I’ve been in business for 18 years so I know how to get them ready and have the postage put on," Smith reports, "this is not my first rodeo."
Inside the store Smith does her best to adhere to the instructions of Ohio Governor Mike Dewine, asking patrons to wear masks and keep a safe six-foot distance from one another. COVID-19 has not affected business to a dramatic degree, as many orders came in via phone even prior to the pandemic.
“I think the time has come," Smith says of the mass call for racial justice, "I see people trying to make change and it’s not an easy process but it's a needed process." When asked if there was a book that was flying off the shelves particularly fast Smith confirmed that Robin DiAngelo's best-seller was in high demand. “It’s called White Fragility," Smith says, "and it’s: Why It's So Hard for White People to Talk About Racism.”
Sylvia Camacho, Grocery Store Owner | Santa Rosa, California, US
*quotes have been translated from the original interview conducted in Spanish.
When the lockdown first took effect in Santa Rosa, California, a small city north of San Francisco, Sylvia Camacho's employees began to dwindle. Camacho and her family have been the owners of Camacho Market, a grocery store and butcher shop, for the past 26 years. Employees were initially most concerned with protective measures, Camacho says, asking her how she would prevent infection, and imploring her to remember that it wouldn't just stop with them. The reluctance of employees to come into work did not pair well with a store that was crowded by nervous shoppers stocking up on toilet paper and food.
"During that time employees were even more nervous to go to work," Camacho explains, "but they had to come in because their families needed it." Two employees have still not returned to work because they are pregnant, and although they haven't yet begun maternity leave, they remain scared for their babies and themselves. Camacho instructed employees to wash their hands as often as possible and to spray all the surfaces that customers could have possibly touched. She herself has returned to the store and works now with a face-mask and gloves.
"We should be grateful to these people, " Camacho says, "the employees that in spite of everything that is happening, they are still working." Those that exposed their health so others could be fed are owed a debt of gratitude that Camacho hopes her clientele will repay by being conscious of the workers and taking care to protect them as well.
Julie Benbenishty, ICU Nurse | Jerusalem, Israel
Julie Benbenishty has only a few minutes for me; she's sharing an early morning cup of coffee with her daughter in some of the little time she has off. When coronavirus arrived in Israel, Benbenishty returned to the ICU at Hadassah Hospital as a nurse, having occupied a more administrative and academic role in recent years. Despite being in a high-risk age group herself, Benbenishty works bedside with COVID-19 patients. Along with her normal shift, Benbenishty is also responsible for coordinating at the national level a randomised control trial for a drug intended to treat the virus.
“You go into the corona [unit] wearing your protective gear and you don’t come out for eight hours," Benbenishty says of her work life, "no one’s telling you not to take a break, but the work is so intense and it takes like ten minutes to undress this protective gear and another ten minutes to get into the protective gear so if you take a break for a half-hour, you’re not really taking a break." That means no eating, no drinking, and no going to the bathroom for a full shift.
Benbenishty explains that wearing protective gear for such a prolonged period of time took a physical effect that was distressing for medical personnel. "I had a very dry mouth, I had very dry eyes, I couldn’t smell, couldn’t breathe, so I was afraid after every shift that I got sick, " she recalls, "but those are just signs of breathing inside that mask and having what we call hypoxia." The lack of oxygen and the effect of breathing one's own carbon dioxide for eight hours created symptoms that mimicked those of COVID-19. It became hard to differentiate, Benbenishty reports, between markers of the virus and markers of a day spent working in the ICU.
Benbenishty says some of the protective gear was spared by medical workers to allow family members of fatal patients to suit up and say their goodbyes. As a mother of three and grandmother of eight, family is important to her. "I can say with great [pride] that my institution, we worked against policy" she reflects, "The policy was not to let any family in because we were afraid we would not have enough protective gear. However, we did let families in; one person in the family was with their loved one when they died.” Outside the ICU, families that were waiting were calling the doctors constantly, Benbenishty says. The relief of having even just that one representative present for the passing of their loved one was well worth the extra equipment she explains, both for the family and the medical staff.