Ultrasound: the misunderstood medical hero still building acquaintance with the developing world
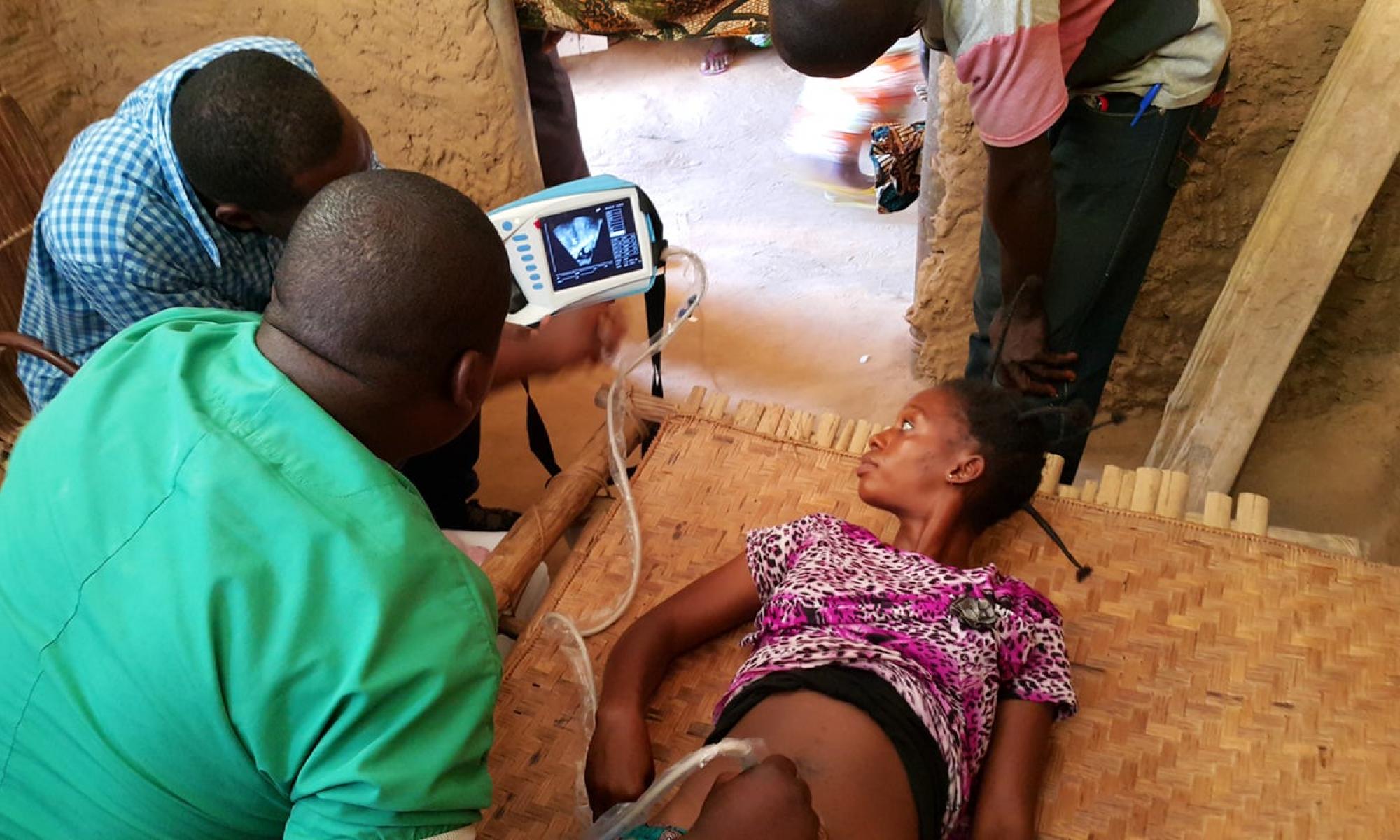
Ultrasound technology is a clinical saviour worldwide. Yet many rural communities in the African continent lack this important extension to clinical observation.
In Sub-Saharan Africa especially, where maternal mortality is extremely high, ultrasound technology has significant benefits to women’s healthcare. Ultrasound can also be used to detect organ-related issues in AIDS sufferers so would prove to be a life-saving technology across the African continent, where AIDS is a devastating epidemic.
In rural African communities, good health is vital for sustaining livelihoods and maintaining food security. In order to carry out the demanding labour of farming practices, secure nutrition and high fitness levels are crucial. Crop production is commonly the main source of income for families who rely on this to fund living necessities. If a household member is ill, often young girls leave school to care for them and help with farm work and other household chores.
It would be difficult to oppose the notion that health is one of, if not, the most important attribute to quality of life. Health issues, in general, are not exclusive to class, ethnicity or social groups. Yet health care services often are.
After ultrasound became an established diagnostic tool in the 1950s, and a carriable device in the 1990s, it became widespread in developing countries. Alongside the technology’s diverse capabilities, its durability, affordability and portable size made it internationally desirable, and accessible to many health centres across the world.
Ultrasound is used for a wide variety of purposes—maternity care, chronic disease management, and disease epidemics are areas where ultrasound has proven to be effective and efficient. Unlike radiology, ultrasound relies on sound waves, making it a safer technique for producing internal images. These images allow for detection and surveillance of a wide range of health issues. Together, ultrasound and x-rays can meet 70-80% of all clinical diagnostic needs. Abdominal, cardiac and renal ultrasounds are common examinations used to view organs, which is important for understanding the numerous organ-related health problems that arise as a consequence of HIV disease. The most common use of ultrasound, however, is for maternity care.
African women living in rural and poor communities are at significant risk of maternal death due to inadequate healthcare facilities and a lack of skilled healthcare professionals. More than half of the world’s maternal mortalities occur in Sub-Saharan Africa, where neonatal deaths are as high as 31 per 1000 live births. Ultrasound’s ability to detect a wide range of foetal anomalies early, such as premature detachment of the placenta, is crucial for reducing the deaths of mothers and babies. Ultrasound scans are capable of finding cysts and ovarian cancers, and are also able to determine the gestational age and whether there are multiple pregnancies, which is vital for allowing good prenatal care and informed decision-making.
A study in Rwanda found that up to 37% of women were given the wrong diagnosis, which would have been corrected through ultrasound pregnancy scans. Another Rwandan study found that ultrasound changed the treatment plan of patients in 43% of cases, and most commonly this change involved arranging a surgical procedure such as caesarean sections or biopsies of found masses. Without ultrasound, women’s risk of fatality during pregnancy is heightened by the inability of healthcare professionals to understand their individual conditions and needs.
The health and wellbeing of mothers and offspring give families a better chance to generate income, as women in rural communities play crucial roles in farming, trading and raising children. The significance of women in crop production ought not to be undervalued as women in Sub-Saharan Africa are responsible for 60-80% of agricultural labour.
What are the challenges?
While ultrasound is a valuable piece of technology that has been implemented in health centres across the globe, many African clinics lack clinicians that are properly trained in the operation of ultrasound machinery, which is an issue compounded by the lack of accessible training services in these regions. Many health clinics throughout the African continent significantly lack human resources—let alone sonographers. In Senegal, a majority of ultrasound practitioners are unqualified. Ultrasonography training is crucial as the incorrect interpretation of ultrasound scans may lead to unnecessary surgeries that risk the health of patients and waste money and resources.
Approximately 80% of Africa’s provincial hospitals lack conventional electricity supply. While a possible solution is to use battery-operated ultrasound equipment, when the batteries run out of power, they are often left in storage uncharged and unused.
Socio-cultural barriers surrounding ultrasound technology make its integration into the healthcare system of developing nations complex and requires the cooperation of the patients to fully reap its benefits. These barriers include misconceptions that ultrasound is dangerous, or that it is invasive in the sense that it involves some nature of insertion. In rural villages, where electronic technology has not been firmly integrated into cultural activity, it is not easily accepted that ultrasound technology is safe and painless. However, this can be combatted by bringing awareness about ultrasound technology among rural populations.
Pregnant women are more often than not unaware that they have the option of ultrasound scans or are oblivious of the technology altogether. In numerous studies, women who underwent ultrasounds in rural clinics commented that they were not informed during the process about what was happening and the conditions of their foetuses. Communication can go a long way in confronting these issues.
Is ultrasound technology a danger or a saviour? Ultimately good management and correct use of the technology and interpretation of the scans performed by qualified sonographers and trained clinicians have changed the lives of suffering patients. And this improvement in quality of life is more valuable than gold—but it should not have to be as rare.